A little background

Until my mid-fifties, I had been strong, fit and healthy. I had run nearly 200 marathons, and in 2009 competed in the Trans Europe Footrace - nine weeks spent running a 3,000 mile race from the south of Italy to the north of Norway. In the years that followed Trans Europe, my wife Claire and I continued to run in stage races across Europe – mainly in Germany, Ireland and France.
Becoming unwell
But then things started very slowly - almost imperceptibly - to go wrong with my health. Three times I passed out after a hard run. At the time, I couldn’t identify the cause of the horrible feelings, but chalked them up to either undertraining or ageing. Either way, I didn’t like the feeling one bit. Each time, I spent several hours getting back to normal.
Finally I turned to my GP to discuss matters. He was visibly concerned, and sent me for lots of tests. He did not believe this was purely an ageing effect, as my vital signs (pulse, blood pressure, weight, etc.) were good for someone my age.
So we started with blood tests. A little anaemia showed up, but nothing else alarming. Iron pills and Guinness did nothing to change the trajectory. Next, X-rays showed a few shadows on the lungs, but nothing serious. Follow-up MRIs showed nothing which would explain my symptoms. My doctor did scare me a little with his thoughts on the possibility of lymphoma – a form of cancer that begins in infection-fighting cells of the immune system – but my blood tests didn’t support that theory.
So we moved on to my heart – was my trusty ticker beginning to give out after 35 years of running? I was sent to cardiologists who carried out standard tests - ECGs, overnight monitors, CT scans, a catheter angiogram, and finally a treadmill stress test. After only nine minutes, I had to ask the medics to turn off the machine and let me rest on a chair. I knew that something was seriously not right, but it just didn’t feel like my heart was the problem. As it turns out, I was right.
Winter 2018
As winter 2018 approached, things went from bad to worse. I was referred to an NHS neurologist, who whilst not being able to diagnose any specific condition, did accept that something serious was going on. By this time, I now know that my family’s fear was that I was developing some form of early onset dementia. I was beginning to sleep a great deal – up to 18 hours a day – and I was suffering really bad headaches whenever I got out of bed. On top of that, my motor skills were starting to fade. I was becoming clumsy and unstable, confused and forgetful. But I was not “with it” enough to understand what was happening to me. I was easily angered and became socially isolated.
All I knew was that I was being told that I was becoming demented, which I didn’t care for one bit. My mother had died of Alzheimer’s a year previously after her 12-year nightmare with the disease, and the thought absolutely terrified me. But unfortunately my sense of reason and awareness had been compromised to the point where I was making very little sense.
Things got worse and worse. Finally, Claire became truly desperate, and decided to take me to the Accident & Emergency department of the local hospital. After some head scratching on the part of the A&E doctors, I was moved to a geriatric ward, and given another series of tests.The doctors were concerned about the possibility of brain tumours or possibly cancer, but those tests came back negative… phew. But I felt terrible, mentally and physically. How had I ended up here? My memory of the two weeks I spent in that hospital bed is as fragmentary as shards of broken glass.
During this hospital stay, my family spent lots of time surfing the web, searching for diagnoses which matched my symptoms. The internet became a tool in their hands, which ultimately helped to save my life. They alighted upon a condition called Cerebrospinal Fluid (CSF) Leak, which matched my symptoms precisely. They also found a Neurology Professor at Cedars-Sinai Hospital in Los Angeles, the man who ultimately saved my life.
But before that...
The next stop in the journey, after review by my consultant neurologist, was Charing Cross Hospital, which had more advanced radiology and surgical options than the local hospital. Before that happened, I had spent a miserable Christmas with my family, sleeping constantly and becoming less and less aware of my surroundings. Headaches were a constant reminder to lie down, which in turn led to more hours of sleep. I was in a very dark and scary place and I knew I didn’t want to live like this.
In January 2019, we arrived at Charing Cross. I had another brain MRI, and this clearly showed that my brain was sagging down into my spine. It was generally agreed that this was caused by a CSF leak – fluid was leaking from somewhere, reducing the CSF pressure in my skull and thus allowing this sagging. The doctors thought that the fluid leak may have been caused by an osteophyte which had shown up on my spinal X-rays, a bone spur on a vertebra which had rubbed against the dura mater, thus allowing fluid to leak. But the radiology at their disposal didn’t allow them to confirm that theory. As it later turned out, the “bone spur theory” was a red herring. It was not the cause of my spinal fluid leakage.
Unsuccessful treatment
Over the course of several weeks, two different remedies to reduce brain sag were attempted - epidural blood patches (EBPs) and caffeine infusions. An EBP is a procedure which takes a quantity of the patient’s own blood, and injects it into the spinal column, using an epidural injection. My anesthesiologist's first attempt at an EBP was completely unsuccessful and it did also make me violently sick. After several horizontal hours I felt no better.
Then a caffeine infusion was tried. (Caffeine, it is suspected, increases the body’s production of cerebrospinal fluid.) It did not appear to make any difference in my case either. I confess to having little recollection of this particular treatment; I was lost at this point.
A few weeks later, the anesthesiologist was reluctantly persuaded to try another EBP. This time – bingo! By injecting into a different part of my spine, the patch relieved the headache symptoms almost immediately, and swung me from depressed and somnolent to happy and manic! I couldn’t sleep, couldn’t stop talking and felt that I had recovered.
But not so fast. Within ten days or so, the old symptoms started to return. More headaches, more instability, more sleep, and more craziness. In retrospect, it is clear that the EBP had “topped up” the fluid in my dura, thus enabling my brain to refloat. But as soon as the on-going leak had done its worst, my brain re-sagged and I was back to where I started.
So, by this point, the doctors knew from MRI imaging that my brain was sagging into my spine due to a CSF leak. Unfortunately, they could not work out why – or where – I was leaking fluid. I was slowly deteriorating. Claire had confiscated my car keys, to prevent me from driving and potentially causing death and destruction on the roads. She also took and hid my passport, so that I could not take a long-planned running holiday to Goa. I was confused and angry at this loss of independence, control and fun. Nothing was making sense to me. I was descending further into madness.
At the next meeting with our neurology consultant, he floated the idea of flying to the US for treatment. He knew that Claire was American, and thought we might have US medical insurance, but sadly we didn’t. But the bottom line was that he did not believe that the NHS had the ability to “fix” me. He suggested Johns Hopkins hospital in Baltimore, but Claire discovered that they had a four month waiting list for treatment. Duke hospital in North Carolina had similar issues. Luckily Claire managed to connect with Cedars-Sinai Hospital in Los Angeles. She sent copies of my MRI scans to Cedars-Sinai, and a quick review there concluded that I was in very bad shape. The neurosurgeon moved his schedule around, and agreed to see me as a matter of urgency within a month. He was confident that he could cure my brain sag. The eye-wateringly high six-figure price of treatment seemed like our only option, and so Claire grabbed his offer in an instant.
When we arrived in Los Angeles airport, I had to be pushed around in a wheelchair. Everything seemed to have stopped working. This was definitely not fun. How does a healthy, sporty 54 year old morph into a geriatric 64 year old? The answer, it appears, is quite rare and tricky to fix.
Diagnosis and treatment in Los Angeles
Within three days, my family members and I had a meeting with the neurosurgeon. We discussed my state of health at some length during my initial consultation.
By this point, I had plenty of symptoms to put on the table:
• My vision was blurry and “foggy”, especially when behind the wheel of a car.
• Hearing was difficult with the constant ringing of tinnitus in my ears.
• I had lost my sense of taste and smell. Food had ceased to be enjoyable. My throat was compromised by the downward pressure of my brain, and so swallowing, speech and coughing became constant issues.
• I was hypersomnolent – meaning that I could sleep for 18 or more hours a day. Getting up from a recumbent position brought on terrible, grinding headaches which could only be relieved by lying back down again.
• I sneezed a great deal, which caused terrible head and eye pain every time.
• My sense of balance and stability when walking was completely compromised.
• Any exertion caused breathlessness, and a weird feeling of heart arrhythmia.
• Oh yes, and I was increasingly having problems with constipation and urinary release. What joys!
But the single most concerning problem was dementia. I was some ways down the road to madness.
After due consideration of this litany of problems, the doctor gave his opinion of my condition, and explained what he planned to do about it. This was the first time a medical professional had uttered the words “frontotemporal dementia” to me. His diagnosis hit me like a rock. It had become official – I was actually mad. I was told that I was to be MRI’d again, to confirm the current status of my brain sag. Then, under general anaesthesia, I would receive something called digital subtraction myelography, a very precise scan of my spine to determine the exact site of the leak. Slightly worryingly, one of the necessary parts of the procedure was stopping my heart and breathing, in order to get the sharpest image possible. Two days later, again under general anaesthesia, they would perform a laminectomy on the vertebrae next to the site of the leak, to allow access to the dura. This part of the procedure would last for four hours.
Even in my confused state, it was clear to me that this doctor knew exactly what he was doing. Only later, weeks after the surgery, did I come to realise that this set of procedures was extremely complex, and not without risk. I found out that he had carried out similar procedures on more than a thousand patients with my kind of neurological impairment, many more than any other neurosurgeon in the world. It’s always nice to know that the person wielding the knife has true experience bona fides.
Recovery
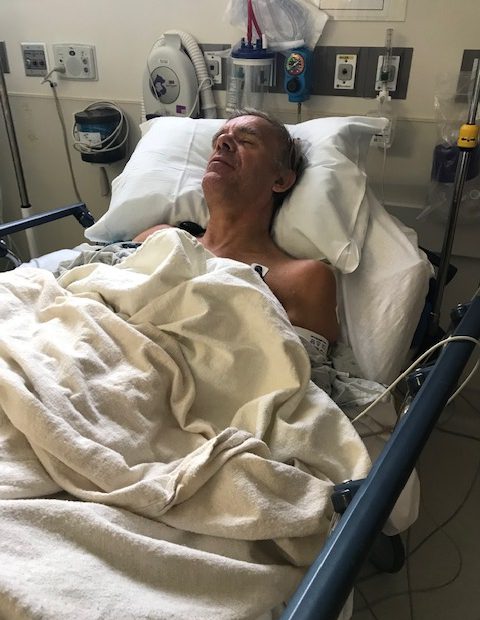
Within a week of arriving in Los Angeles, I found myself lying in a hospital bed recovering from scans, anaesthesia and surgery. My back was miserably sore, but I had made it through without any problems. After two nights at Cedars-Sinai, under the care of brilliant nurses and doctors, I could feel the fog of dementia starting to lift already. My head didn’t ache. Things were starting to make sense. I was even able to slowly walk back to our hotel with my family, supported by my kids, although I did feel a hundred years old!
It turns out that the cause of my CSF leak had been a dural cyst between the eighth and ninth thoracic vertebrae - which I had probably had since birth - and which had been somehow connected to a venous fistula, a rogue vein which was allowing spinal fluid to escape the dura and into the rest of my body. Surgery involved cutting and cauterising off the fistula, and then placing two aneurysm clips and fibrin glue on the cyst. He seemed confident that his handiwork had stopped any further leakage permanently.
The week after surgery was very tough for me, physically and emotionally. Claire and I were stuck in a hotel room in Los Angeles close to the hospital, waiting to see if my surgery had actually done the trick. The first thing I had to deal with was the incredible soreness in my back. However I tried to lie in bed, my back objected. I didn’t want to move much and risk tearing open the angry scar in my back, but if I lay still, the pain just grew and grew. Sleep was fitful and very uncomfortable.
My next complaint was the effects of anaesthesia and painkillers on my system. From a physical perspective, the chemicals that had been poured into my body twice within three days had made me extremely constipated, which is not a nice feeling. But from a mental point of view, the drugs had turned me into a weepy baby. I would get up and sit in the hotel lobby at 5 a.m. drinking coffee after coffee, sobbing as I listened to old songs which had some peculiar meaning for me. Jackson Browne’s “These Days” made me feel particularly raw, especially the line that goes: “Don’t confront me with my failings, I have not forgotten them.” I found a Nico cover of that song, and that version made the crying even worse. To this day, those songs give me intense flashbacks to LA.
On the upside, the one thing that was recommended as part of my recovery was walking. Tentatively at first, Claire and I started to walk each day to nearby shopping malls and restaurants. It felt absolutely wonderful to be able to walk without stumbling, and to get fresh air. She tracked our “steps” with her GPS device, and each day we went a little farther and longer. After half an hour or so, my back would start to hurt, so we would find a coffee shop and top up my still dramatic caffeine intake.
One of our first “outings” was to get breakfast in a nearby diner recommended by our son and daughter-in-law. It was not a happy experience for me. Due to the sudden re-engagement of my sense of smell, the whole place seemed to reek disgustingly. Fried food had never tasted or smelled so vile to me. I tried to eat some of the food put in front of me, but the overwhelming, heightened smell of the place made it very difficult. So we henceforth confined ourselves to organic cafes and drank smoothies, something I’d never done before. I didn’t really care for them, but at least they didn’t overpower me with a foul odour.
Happy Ending

A week after surgery, a final MRI clearly showed that my brain was floating again, and my cranial nerves, pituitary gland, and all that tricky wiring stuff was getting back to the right size, shape and position. It was clear that this intervention had successfully cured me. I thanked my doctor profusely at our final consultation – it is not often that you get to thank someone personally for saving your life.
We had all learned a lot about neuroscience in the recent weeks and months. When you peek behind the curtain of the human form, you quickly realise how breathtakingly complex yet fragile it all is. My “crazy” symptoms were receding, as my brain cavity refilled with the primordial soup of cerebrospinal fluid.
So, my life continues healthily once again. The “brain fog” has cleared. Senses like smell, taste, appetite, and vision have recovered nicely. And I can finally sleep more normally - eight hours instead of fifteen a night. I can walk without stumbling or falling. Headaches and my painkiller intake is a thing of the past. I can swallow without choking. And I can drive a car safely again. I am remarkably fortunate and will be forever grateful that I could be correctly diagnosed and effectively treated. My wife Claire’s support and advocacy clearly made a life-saving difference to my outcome.
These are excerpts from my recent book “Marathons, Madness and Mastermind”. It describes the difficult CSF Leak journey my wife Claire and I took over a period of four years.
